From silent measles spread to a new gene therapy for deafness, here’s what you need to know about three major health stories today.
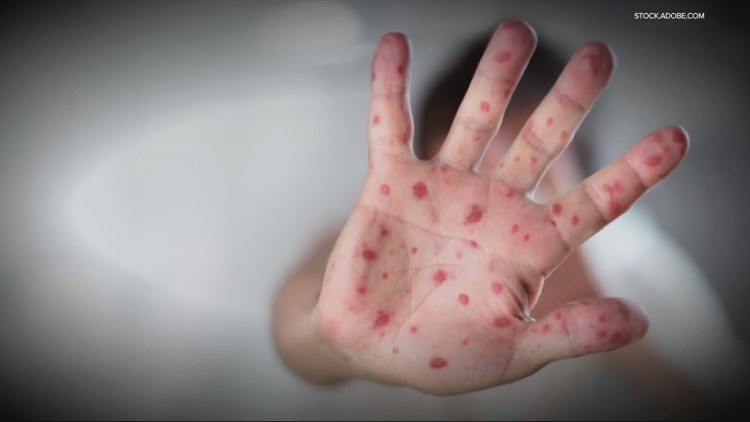
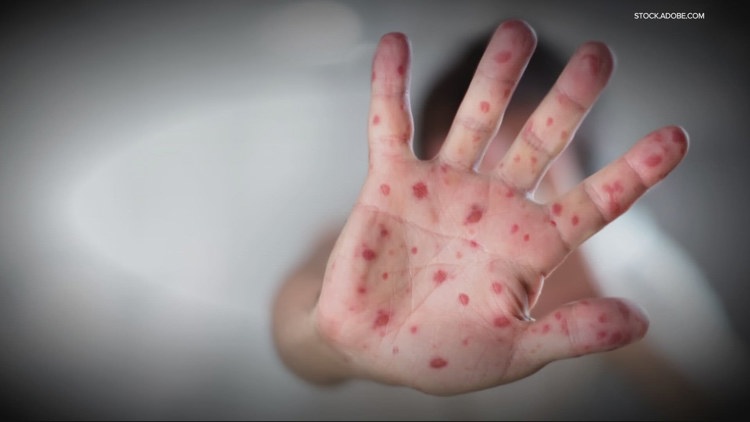
CLEVELAND — The measles outbreak making headlines may be far bigger than the numbers suggest — and new science is raising urgent questions about how the virus spreads before anyone even knows it’s there.
The measles numbers may be just the tip of the iceberg
A major outbreak along the Arizona-Utah border has surpassed 600 confirmed cases, but researchers say the true toll could be more than six times higher. The evidence is coming from two directions — and both are alarming.
The CDC and local health departments have now sequenced more than 1,000 measles virus genomes collected in 2025 and early 2026. That genetic data is confirming something health officials had feared: the virus isn’t just being imported from other countries. It is spreading continuously within the United States — person to person, community to community — in chains of transmission that traditional case reporting has been missing entirely.
Wastewater surveillance tells the same story. In Oregon, testing detected measles at least 100 times between October 2025 and February 2026, even as only six clinical cases were officially reported during that period. Advanced genetic sequencing has also revealed that the virus may have been circulating for weeks — or even months — before the first confirmed case in some outbreaks.
Analysis of 2025 data identified four major outbreaks, each topping 50 cases, that accounted for 73% of all cases that year — many linked to a single rapidly spreading strain.
So why are so many cases going undetected? Health experts point to three overlapping problems: communities with low vaccination rates, patients who refuse testing, and doctors who don’t always test for measles — leaving cases uncounted and chains of transmission unbroken.
The consequences extend beyond case counts. The genetic evidence now points toward continuous endemic transmission, raising serious questions about whether the U.S. can maintain the measles elimination status it achieved in 2000. The Pan American Health Organization is expected to make that determination this fall.
Measles cases surged to more than 2,200 last year — the highest in over three decades. More than 1,700 cases were reported in just the first four months of this year alone.
A landmark gene therapy — and a rare promise on price
The FDA approved the first gene therapy for inherited hearing loss this week, and for the roughly 50 babies born each year in the U.S. with the specific genetic mutation it targets, it could be life-changing.
The treatment, called Otoarmeni, requires only a single administration. In clinical trials, 16 out of 20 children born deaf showed measurable hearing improvement after five months. Of the 12 followed for a full year, five achieved normal hearing.
Treatments for conditions this rare often carry price tags in the millions. But Regeneron, which developed the therapy, has committed to offering it free of charge — calling it a demonstration of biotechnology’s potential. Patients will still be responsible for the cost of the minor surgical procedure required to receive it.
The HPV vaccine protects men, too
A vaccine long associated with cervical cancer prevention in women is showing powerful benefits for men — and a major new study is making the case that boys need to be part of the conversation.
HPV, or human papillomavirus, is one of the most common viruses in the world. Nearly all sexually active people are exposed to it at some point. While most infections clear on their own, some persist — and can lead to cancer years later.
In women, the most recognized risk is cervical cancer. But HPV is also responsible for more than 90% of anal cancers, about 70% of oropharyngeal — or throat — cancers, and more than 60% of penile cancers.
A large new study published in JAMA Oncology found that vaccinated males had roughly half the risk of developing HPV-related cancers compared to those who were unvaccinated — a nearly 46% reduction overall. The protection held across age groups, with those vaccinated between 9 and 14 showing about a 42% lower risk, and those vaccinated between 15 and 26 showing roughly 50% lower risk.
The CDC recommends routine HPV vaccination for preteens starting at age 11 or 12, with the series available as early as age 9. The American Academy of Pediatrics similarly recommends starting between ages 9 and 12 — before any potential exposure. Catch-up vaccination is recommended through age 26, and adults 27 to 45 can discuss options with their provider. The vaccine is approved for people ages 9 through 45.
💌 Mantente al Día con lo Último del Entretenimiento Latino
Recibe noticias exclusivas de celebridades latinas, chismes virales, belleza, moda y entretenimiento — directo en tu correo.
Sin spam. Solo lo mejor de Atlanta Latinos Magazine.